The Jackson Care Connect Member Handbook is available in the following languages:
Or read the handbook in large print:
If you would prefer a printed copy of the handbook, call Customer Service at 541-500-0567 or toll-free at 855-722-8208 (TTY 711). There’s no charge, and you’ll receive a copy within five business days. You may also receive a copy in large print or in languages other than English.
OHP Bridge is a new Oregon Health Plan (OHP) benefit package that covers adults with higher incomes. People who can get OHP Bridge must:
- Be 19 to 65 years old;
- Have an income between 139 percent and 200 percent of the federal poverty level (FPL);
- Have an eligible citizenship or immigration status to qualify; and,
- Not have access to other affordable health insurance.
OHP Bridge is almost the same as OHP Plus.
The two benefit packages are almost the same. There are a few things that OHP Bridge does not cover. To learn more about what OHP Bridge does not cover, please see the table below.
| OHP Bridge covers | OHP Bridge does not cover |
|---|---|
|
|
OHP Bridge is free to members. Just like OHP Plus, OHP Bridge is free to members. That means no premiums, no co-payments, no coinsurance, and no deductibles.
OHP members with income changes may be moved to OHP Bridge automatically. If you have OHP now, you don’t have to do anything to get OHP Bridge. If you report a higher income when you renew your OHP, you may be moved to OHP Bridge.
People who do not have OHP right now can apply for OHP Bridge.
Go to Benefits.Oregon.gov to apply. You can also use that link to find information about how to apply in person, get application help, or to get a paper application. To apply over the phone, call the ONE Customer Service Center at 1-800-699-9075 (toll-free, all relay calls are accepted).
Below are some of the most common forms used by members. Click on the links to open the forms in PDF format.
- Direct Member Reimbursement form: prescription drugs
- Member COVID-19 At Home Test Reimbursement form
- Authorization to Release Personal Health Information (PHI) form
- Member Request to Review Claims Records form
- Adolescent Well-Care Incentive form
- Adolescent Well-Care Incentive form (Español)
- Appointment of Representative form: English | Spanish
- Complaint and feedback form: English | Spanish
When you become a Jackson Care Connect member, we’ll mail you a Member ID card within 30 days. Your Member ID card lists your PCP. It also lists important contact information. The card looks like this:
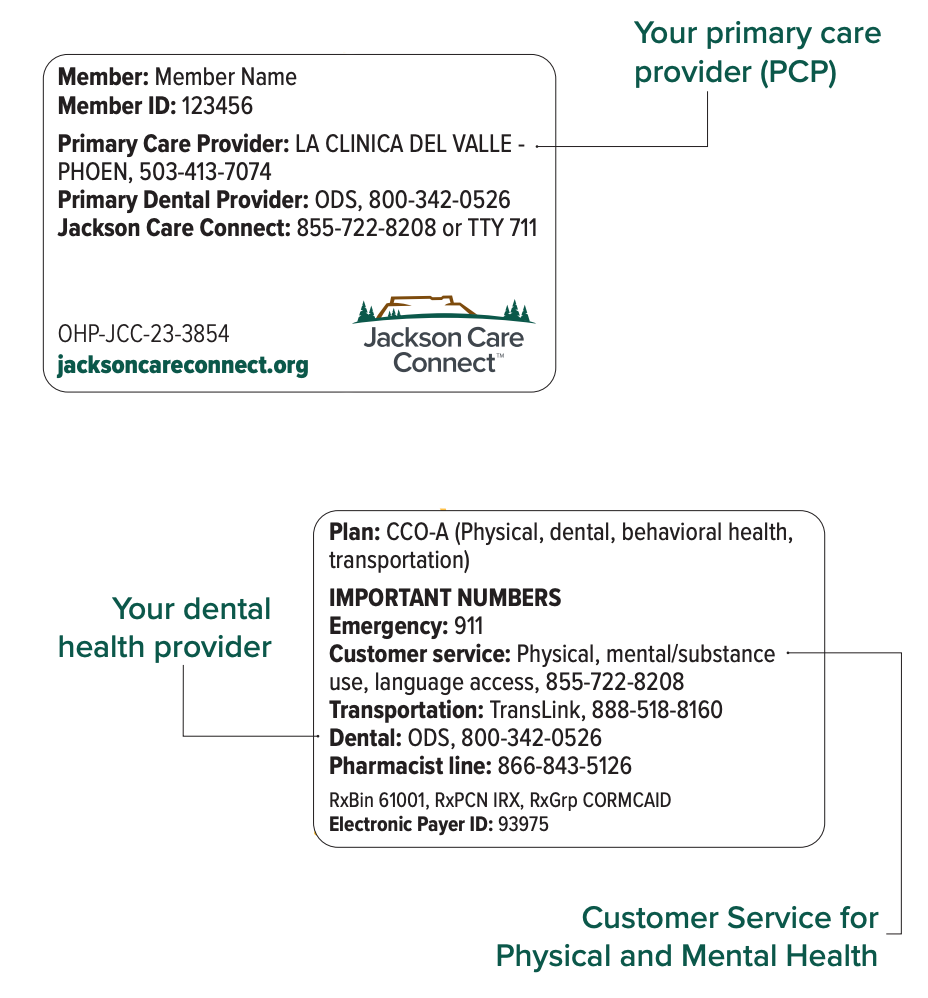
Take your Jackson Care Connect Member ID card to all your physical, dental and mental health care appointments and to the pharmacy when you fill a prescription.
Reasons to take your card with you:
- It’s easier to check in for appointments.
- It’s easier to get medicine at a pharmacy.
- Your provider will know whom to bill.
- Providers use information on Member ID cards to make sure you have benefits with us.
If you or a family member changes PCPs, we’ll automatically send you a new Member ID card. If you lose your card, call Customer Service and we’ll send you a new one.
If you need an interpreter for visits or phone calls to your (or your child’s) provider’s office, you are legally entitled to this service free of charge. When you join Jackson Care Connect, you may receive a Preferred Language card. The card informs your provider’s office of your spoken language and will show the language you selected on your Medicaid application. Please show this to your provider to receive interpretation.
For phone interpretation, call Customer Service when you are at the doctor, dentist or pharmacist, or while you are making an appointment.
Please call Customer Service if you have any problems getting an interpreter.
As an OHP member, you will be:
- Treated with dignity, respect and privacy.
- Free to choose your primary care provider (PCP).
- Urged to tell your PCP about all your health concerns.
- Able to have a friend or helper come to your appointments, and an interpreter if you want one.
- Told about all of your OHP-covered and non-covered treatment options.
- Allowed to help make decisions about your health care, including refusing treatment, without being kept away from other people or forced to do something you don’t want to do.
- Given a referral or second opinion, if you need it.
- Given care when you need it. 24 hours a day, seven days a week.
- Free to get mental health and family planning services without a referral.
- Free to get help with addiction to tobacco products, alcohol and drugs without a referral.
- Given handbooks and letters you can understand.
- Able to see and get a copy of your health records.
- Able to limit who can see your health records.
- Sent a Notice of Action letter if you are denied a service or there is a change in service level.
- Given information and help to appeal denials and ask for a hearing.
- Free from any form of restraint or seclusion (isolation) that is not medically necessary or is used by staff to bully or punish you. Staff may not restrain or isolate you for the staff’s convenience or retaliation against you. You have the right to report violations to Jackson Care Connect and/or the Oregon Health Plan.
- Allowed to make complaints and get a response without a bad reaction from your plan or provider.
- Free to ask the Oregon Health Authority Ombudsperson for help with problems. You can reach them at 503-947-2346 or toll-free 877-642-0450 (TTY 711).
As an OHP member, you agree to:
- Find a doctor or other provider you can work with and tell them about your health.
- Treat providers and their staff with the same respect you want.
- Bring your Member ID card to appointments, tell the receptionist that you have OHP and any other health insurance, and let them know if you were hurt in an accident.
- Be on time for appointments.
- Call your provider as soon as possible if you can’t make it to an appointment.
- Have yearly check-ups, wellness visits and other services to prevent illness and keep you healthy.
- Follow your providers’ and pharmacists’ directions or ask for another choice.
- Be honest with your providers to get the best service possible.
- Call OHP Customer Service when you move, are pregnant or are no longer pregnant.
Jackson Care Connect takes fraud, waste and abuse very seriously. We comply with all applicable laws, including the State and Federal False Claims Act. Examples of fraud, waste and abuse include:
Provider fraud:
- Billing for services not rendered
- Altering medical records
- Use of unlicensed staff
- Drug diversion (for example, dispensing controlled substances with no legitimate medical purpose)
- Kickbacks and bribery
- Providing unnecessary services to members
Member fraud:
- Falsifying information
- Forging or selling prescription drugs
- Using transportation benefits for non-medical business
- Adding an ineligible dependent to the plan
- Lending or using another person’s insurance card
- Identity theft
If you suspect your benefits aren't being used correctly or want to report a case of fraud, waste or abuse, contact EthicsPoint at 888-331-6524. You can also file a report online at EthicsPoint.
The Oregon Health Authority (OHA) sends you a coverage letter that shows your:
- Benefit package
- Coordinated care plan name
This letter gives information for everyone in your household who has an Oregon Health Plan (OHP) ID card. You do not need to take this letter to your health care appointments or pharmacies. OHA will send you a new coverage letter if you ask for one or if your coverage changes.
OHA sends you one OHP ID card that has your name, Member ID number and the date the card was issued. All eligible members in your household receive their own OHP ID cards.
Keep your OHP ID card in a safe place. OHA only sends a new card if you change your name or ask for a new card. If there are any issues with your OHP ID card, call OHP Customer Service right away at 800-699-9075 (TTY 711).
There are three ways to contact OHP for questions or to make updates to your current information:
1. By telephone (toll-free): 800-699-9075
Members can call OHP to do any of the following:
- Change your address, phone number, family status, CCO or other information
- Replace a lost OHP Card
- Check the status of your application
- See if you or your children are still covered by OHP
- Change plans
- Solve a problem or make a complaint
- Get an OHP Handbook
2. By email: oregonhealthplan.changes@state.or.us Your email must include your full name, date of birth, Member ID number and phone number.
Existing members can email OHP to change your address, phone number, family status, CCO or other information. Note: The email address is for changes only.
3. Online: Most OHP members can report changes online at ONE.Oregon.gov. The online site supports the following browsers. (If you don't know your browser version, click your browser's Help menu, then click About.)
- Windows (PC): Internet Explorer 11, Internet Explorer 10, Internet Explorer 9, Internet Explorer 8, Firefox 39.0 and 43.0 and Chrome 43.0 and 44.0.
- Macintosh: Firefox 39.0 and 43.0 and Chrome 43.0 and 44.0. Safari is not supported.
- Smartphone browsers are not supported.
Need help?
- Learn how to set up your online account. English | Español
- Learn to use your online account dashboard. English | Español
- Watch a five-minute overview of the Applicant Portal.
You must apply every 12 months to keep your Oregon Health Plan (OHP) coverage. OHP sends you a letter about how to keep your membership. It will include a form for you to fill out and return. You can also create an account at ONE.Oregon.gov to apply or update your information.
We also will contact you near your renewal date. We’ll send you a list of places and phone numbers where you can get help to apply.
OHP assistors are available at these locations.
Oregon Health Authority: 1-800-699-9075
Best times to call OHA are Tues-Fri at 7 am. Avoid calling Mondays, as there are long wait periods.
Jackson County in-person assistance:
Limited in-person assistance and phone assistance available. Call for appointment.
Ontrack Rogue Valley
30 W Main Street
Medford, OR 97501
Office: 541-200-2407
Languages Spoken: English
Unete, Center for Farm Worker Advocacy
607 W Main Street
Medford, OR 97501
Office: 541-245-1625
Languages Spoken: English, Spanish
Jackson County phone assistance:
All in-person assistance at these locations is closed. Phone appointments available only.
ACCESS
Phone: 541-601-6793
Languages Spoken: English, Spanish
La Clinica (all clinic locations)
Phone: 541-535-6239
Languages Spoken: English, Spanish
Providence Medford Medical Center
Phone: 503-215-4300
Languages Spoken: English
Rogue Community Health
Languages Spoken: English, Spanish
Medford: 541-773-3863
White City: 541-826-5853
Ashland: 541-482-9741
Butte Falls: 541-842-7799
Prospect: 541-560-1180
How to make a complaint or grievance
If you are unhappy with Jackson Care Connect, your health care services or your provider, you can complain or file a grievance at any time, for anything other than a denial of service. Your provider or authorized representative may also file a grievance on your behalf with your written consent.
We will try to make things better. Just call Customer Service at 855-722-8208, TTY 711 or send us a letter to the address on page 55 of your member handbook, available on this page.
You can also fill out a complaint and feedback form here:
Jackson Care Connect will work to resolve your complaint or grievance as quickly as your health condition requires. If we need more than five business days, we will send you a letter to let you know why. You will receive a final answer within 30 calendar days. We will not tell anyone about your complaint unless you ask us to.
You can also file a complaint with:
Oregon Health Authority (OHA)
Please call the OHP Client Services unit (CSU) toll free at 800-273-0557 or OHA’s Ombudsman at 503-947-2346 or toll free at 877-642-0450.
Appeals and hearings
If we deny, stop or reduce a medical service your provider has ordered, we will mail you a Notice of Action letter explaining why we made that decision. You have a right to ask to change it through an appeal and a state fair hearing. You must ask for an appeal no more than 60 days from the date on the Notice of Action letter. You can ask for a denial notice that shows a service is not covered if:
- You did not receive a written notice of denial, or;
- Your provider tells you that you will need to pay for a service that is not covered.
For full instructions on the appeals process, please see page 54 of your member handbook, available at the top of this page.
Provider Appeals
Your provider has a right to appeal for you when their physician’s orders are denied by a plan. You must agree to this in writing. Instructions for this process can be found on page 55 of your member handbook.
.tmb-ze-200-120.tmb-thumbnail.png?Culture=en&sfvrsn=abfd8dd6_1)